Local healthcare workers still experience burden of COVID-19
The Lewiston-Clarkston Valley has dramatically eased up on COVID-19 protocol since the disease first appeared in the community in early 2020. But healthcare workers here are still experiencing the weight of the virus’ impacts. The recent arrival of the delta variant continues to overwhelm those who are working directly with the illness and other patients needing medical care.
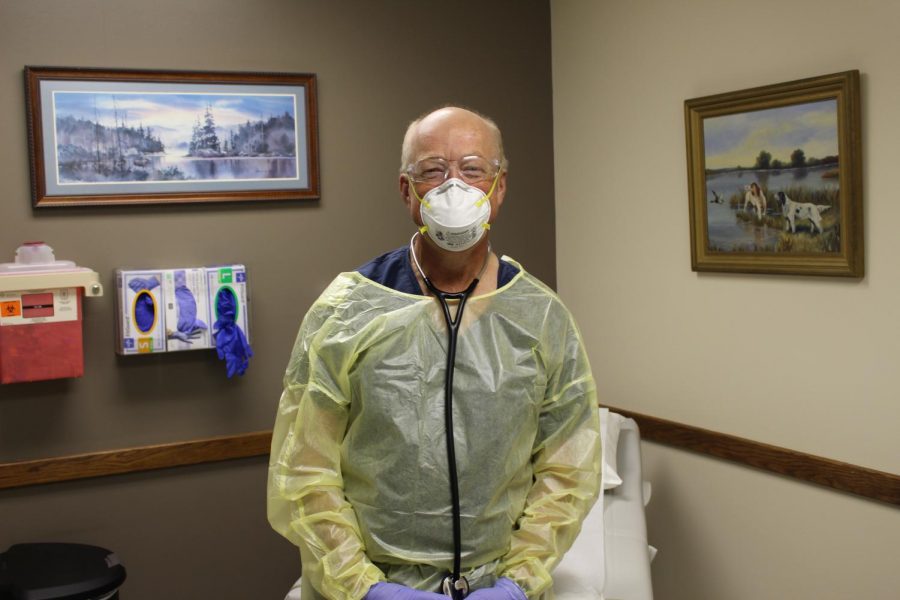
Donald Greggain is a family physician at Southway Family Medicine in Lewiston, and he’s also director of the COVID-19 Respiratory Infection Clinic for St. Joseph Regional Medical Center here. He confirms that local residents in the younger demographic, including the 20- to 25-year-old group and children, are getting very ill from the virus. People with the delta variant tend to be younger, sicker, and need hospitalization earlier, he said. And this has led to more of the overall public being sick than a year ago.
Greggain found several correlations for the rise in cases. The delta variant affects younger people more than the original COVID-19variant, but the community as a whole is also less cautious than before, he said. Masks are less common and social distancing is rarely practiced here, creating a larger viral load than individuals were exposed to last year. He added that locals who are getting ill, hospitalized, and dying of COVID-19 are overwhelmingly from the unvaccinated group.
Healthcare workers in the Lewiston-Clarkston Valley have experienced many challenges since COVID-19 became prevalent here. One difficulty with the pandemic has surfaced in the process of testing potential patients. Greggain’s office still gives COVID-19 tests on Thursday afternoons from 3-5:30 p.m., in addition to providing its regular services.
The lengthy process of testing includes patients waiting in their cars and coming into the clinic one person at a time. Then each patient uses a different exam room, with medical staff changing personal protective equipment each time. The room previously used is sterilized and cleaned using viruscide.
Meanwhile, local hospitals are out of beds and nurses to care for patients, Greggain said. This means that patients, both those experiencing COVID-19 and those in need of other hospital care, are being sent to places as far away as Reno, Nevada, or Sacramento, California. Greggain mentioned one emergency room doctor who phoned 83 hospitals to find an empty bed for someone with a non-COVID-19-related illness.
Greggain said he also feels concerned for those who might avoid care by staying away from medical offices. He worries about those who are unable to get care because specialists and hospitals are preoccupied with COVID-19 patients.
He recognized that mental health has experienced a decline in the community. Social isolation, as well as polarizing views on vaccines and COVID-19, have taken a toll on individuals. This has contributed to a rise in use of less helpful coping techniques, such as drugs and alcohol.
Greggain recommended reaching out to others, but cautioned that people should still try to maintain a pandemic “social bubble.” He encouraged the practice good social hygiene, especially when a person is uncertain of another person’s COVID-19 vaccination status. He said he hopes people will be willing to admit when they need help and seek support.
Healthcare workers are tired and fatigued from the past year and a half of a pandemic, he said. Many are asking that community members get vaccinated to stop the spread of the virus. The only way to lower the number of infected people, and in turn decrease the workload for healthcare workers, is thorough and comprehensive population vaccination, according to Greggain.
“It just saddens our hearts, those of us that are working in this, to know that we have an answer . . . and it doesn’t need to be this tragic,” Greggain said. “But we have a reticence for people to believe in the science and in the legitimacy of vaccinations. That’s a huge heartbreak for those of us who have watched this vaccination being developed over the last 12 years.”
Greggain pleaded with locals to get the COVID-19 vaccine, adding that people who experience negative reactions to a flu shot and other vaccines should not expect a negative reaction to the COVID-19 vaccine.
“I recognize that people don’t like being told what to do, [and they] particularly don’t like being told by a government to do anything,” Greggain said. “But [if] it’s because you ideologically disagree with the politics, well, look past the politics. . . . The virus doesn’t care. It just knows it’s an RNA organism looking for a host.”
“For all of the people that stood on the corners or on their front walks and cheered and applauded front line workers a year ago, when we didn’t have a vaccine, if those same people are not vaccinated now, then all of the cheering that they did last year means nothing,” Greggain said.